Could New TAVR Volume Criteria Open the Competitive Floodgate?
Two recent developments are important for those hospitals monitoring Transcatheter Aortic Valve...
Occasionally, CFA will highlight a few significant news articles on cardiovascular topics -- clinical or organizational.
Reprinted below are four interesting news items we feel worthy to highlight. For full information, the links to the original news sources are included. We have included our interpretation of the organizational implications of each item.
The global market for transcatheter treatment of the mitral and aortic valves is expected to double over the next five years, according to a new report from BCC Research. The industry analysis projects an increase from $4 billion in 2018 to $8 billion in 2023, at a compound annual growth rate of 14.8 percent. Transcatheter mitral valve repair (TMVR) accounted for just 12 percent of transcatheter aortic or mitral procedures in 2017, according to the report, but are expected to grow faster over the next few years than the more established field of transcatheter aortic valve replacement (TAVR). In 2023, BBC research predicts TMVR will account for 22 percent of the segment while TAVR will claim the other 78 percent—down from 88 percent in 2017. But market barriers exist as well, according to BCC Research analyst Ritu Thakur Dangi, BAMS, who authored the report. The high cost of heart valves, concerns over the surveillance and long-term durability of artificial valves, reimbursement issues and regulatory approval processes could hamstring growth, she told Cardiovascular Business.
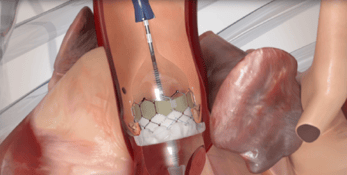
Two trials evaluating transcatheter aortic valve replacement (TAVR) in low-risk patients haven’t just shifted the TAVR versus surgical AVR discussion. They’ve completely flipped it, said experts here at the American College of Cardiology’s scientific sessions. “It used to be that TAVR was really a therapy that was appropriate for patients who were not good candidates for surgery,” said Martin B. Leon, MD, lead author of the PARTNER 3 low-risk TAVR trial. “We think that’s turned around and that probably TAVR should be the therapy considered and surgery should be used in patients that are not good candidates for TAVR.” Leon presented results of the randomized trial March 17 at ACC.19, a day after they were published online in The New England Journal of Medicine.
Implications – TAVR/TMVR continues to be a growth area for select providers who can produce sufficient volume to justify the clinical/organizational/financial commitments required. As CFA has written, providers with small structural heart programs that rely on SAVR will continue to see the erosion of valve surgery volume as patients migrate to regional TAVR/TMVR centers of excellence – unless/until federal regulatory and reimbursement policies change. Also see our blog, Low-Volume Cardiac Surgery Programs: Mitral Valve Surgery Trends and Implications, posted 3/15/19.
Vimal Ramjee, MD, senior staff cardiologist at the Chattanooga (Tennessee) Heart Institute, writes enthusiastically in Cardiovascular Business Practice Management that, while he doesn’t have a “magic 8 ball,” Although no test can predict the future, the coronary artery calcium scan (CACS) is near the front of the pack in this regard. Why? Because a coronary artery calcium score outperforms all other risk factors used today in predicting future cardiovascular events. Clinically it’s a winner, so it’s no surprise that the latest American College of Cardiology/American Heart Association practice guideline on managing cholesterol added a class IIA recommendation to include CAC testing for intermediate-risk individuals who have an uncertain need for primary prevention statin therapy (J Am Coll Cardiol, online Nov. 8, 2018). Though CACS was already widely used, its formal inclusion in the guideline will likely increase its use in cardiovascular and primary care practices nationally.”
Implications – CACS is proving to be an effective and extremely important screening and diagnostic tool as part of an organized marketing campaign for hospital CV programs. CFA has experience with hospitals that have dramatically increased brand awareness, regional/local patient referrals, physician in-office visits, and down-stream cardiology diagnostic and treatment business from these efforts. Also see our blog, CT Coronary Artery Calcium Scoring Revisited: One Hospital’s Successful Cardiac Screening Program, posted 12/6/18.
The average cardiovascular surgeon drives nearly $3.7 million in net revenue each year for a hospital system, the most among 18 physician specialties included in a survey of hospital chief financial officers. Invasive cardiologists weren’t far behind, ranking No. 2 at almost $3.5 million per year. The survey, conducted by the physician search and consulting firm Merritt Hawkins, featured responses from 62 hospital CFOs or financial managers, who provided data on 93 separate hospitals. When pooling all physician specialties, the average revenue generated was almost $2.4 million, the highest of the seven times this survey has been conducted and a 52 percent increase from the most recent report in 2016 ($1.56 million). Invasive cardiologists were one of the groups that made a big jump, driving $2.4 million in hospital revenue in 2016 and almost $3.5 million in 2019. “These results suggest that value-based delivery models have not reduced the volume and/or the cost of physician specialty care, and that such efforts may be trumped by both the continued prevalence of fee-for-service payment models and, in particular, by increased utilization of physician services driven by population aging,” according to the report.
Implications – All hospitals recognize the importance of cardiovascular services to their bottom line. Increasingly, competition for cardiovascular surgeons and invasive cardiologists is intensifying, given their overall monetary contribution and scarcity in the marketplace. Programs are built around these specialists and they remain the primary critical building block for success in virtually all marketplaces. Recruiting and retaining the right physician continues to be a critical and increasingly challenging endeavor for any program.
After being ranked as one of the lowest performing hospitals in the country for adult heart surgeries in August 2018, University Hospital in San Antonio is retooling its heart care program, according to San Antonio Express-News. In August, the Society of Thoracic Surgeons gave the hospital one star, its lowest ranking, for overall performance in aortic valve replacement surgery as well as for combined aortic valve and coronary artery bypass surgery. The hospital's scores improved slightly in January after data from the first half of 2018 was included — it was bumped up to two stars for aortic valve replacement surgery. However, University Hospital remains among the lowest ranking hospitals for heart surgery. The hospital's heart surgeons did note there are certain factors, such as socioeconomic and insurance status, that are not included in STS ratings. University Hospital is a safety net hospital and thus may accommodate more uninsured patients or patients with more comorbidities. But the surgeons have acknowledged they are unsatisfied with the scores.
Implications – While price transparency may be the au current issue, the bedrock of quality outcomes and its transparency is also a critical issue for hospital cardiovascular programs. One could argue that it shouldn’t take a one-star STS rating for any hospital to recognize it has a quality outcomes problem and spur it on to action, but the increasing transparency in outcomes means that every hospital must begin to aggressively address overall performance in quality outcomes as well as pricing. Low volumes, particularly for some specific types of cardiac surgery (particularly structural heart surgery), contributes to this challenge.
If you are interested in learning more about any of these important issues or in cardiac services strategic development, service expansion and/or other programmatic needs for cardiovascular or other services, please contact CFA at (949) 443-4005 or by e-mail at cfa@charlesfrancassociates.com.
Two recent developments are important for those hospitals monitoring Transcatheter Aortic Valve...

Hospitals with small to medium-sized cardiac valve surgery programs need to know that the era of...