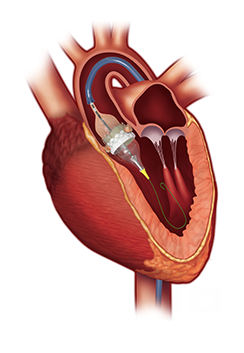
CMS Final Rule Released Ending the Mandatory Cardiac Bundled Payment Initiative
The Centers for Medicare and Medicaid Services in a final rule released Thursday, November 30, 2017, closed the loop on its proposed cancellation of the cardiac bundled payment models.