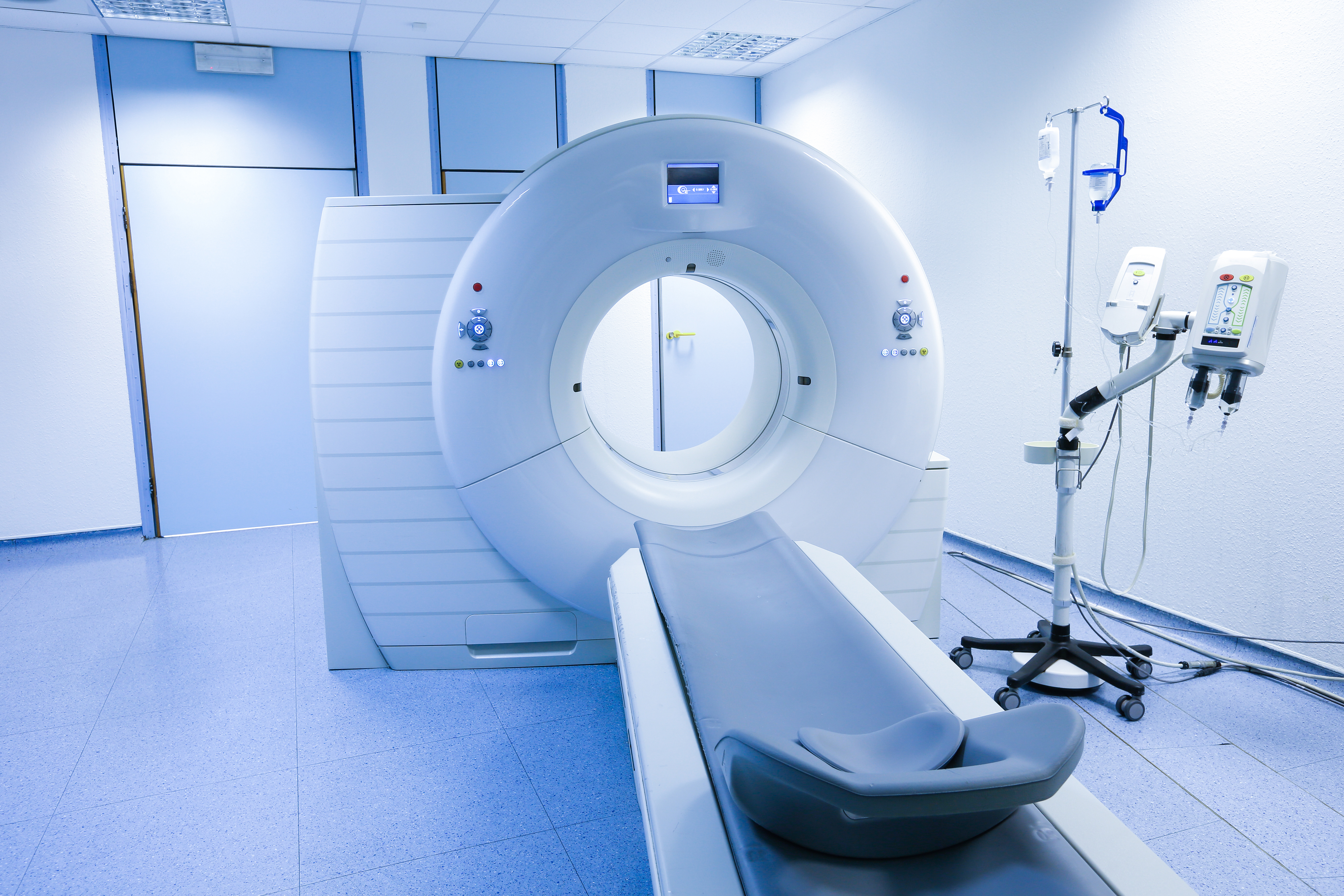
Coronary CT Angiography Finally Gets Its (Official) Due
While cardiac computer tomography (CCT) has been around for twenty years, its widespread adoption has been measured, while its utility and applicability have been continually debated and refined.






















































 I came in from my morning three mile walk to be greeted by this e-mail headline: Most U.S. adults do not know exercise guidelines for preventing heart disease. I wasn’t shocked.
I came in from my morning three mile walk to be greeted by this e-mail headline: Most U.S. adults do not know exercise guidelines for preventing heart disease. I wasn’t shocked.
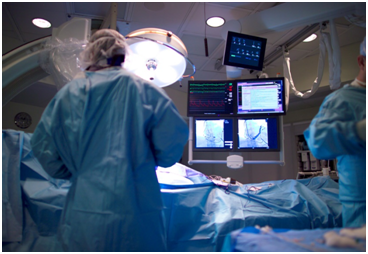



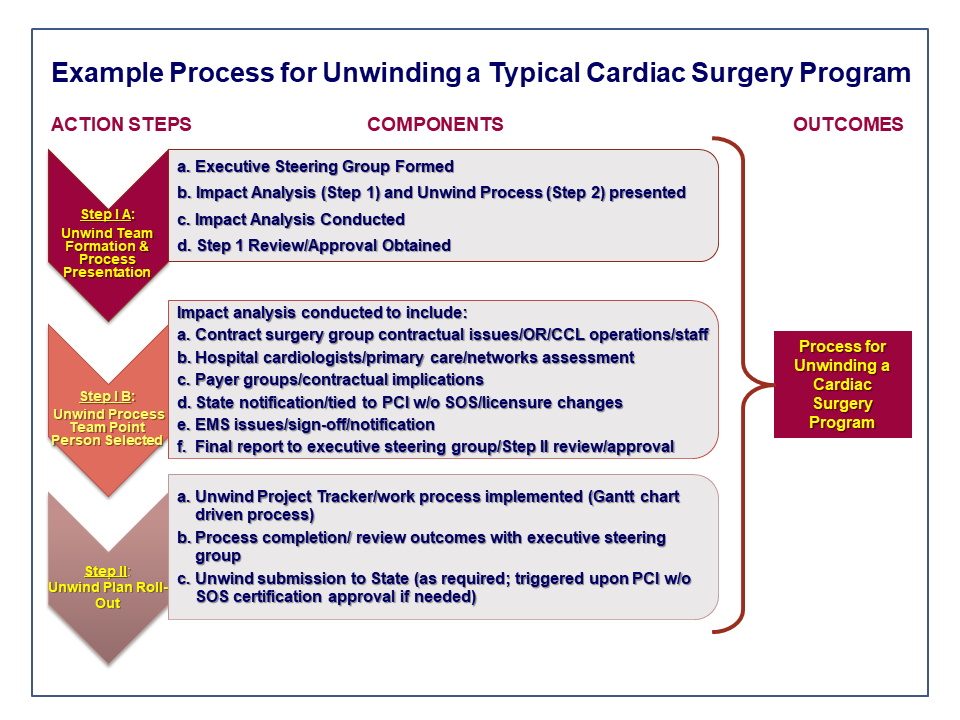
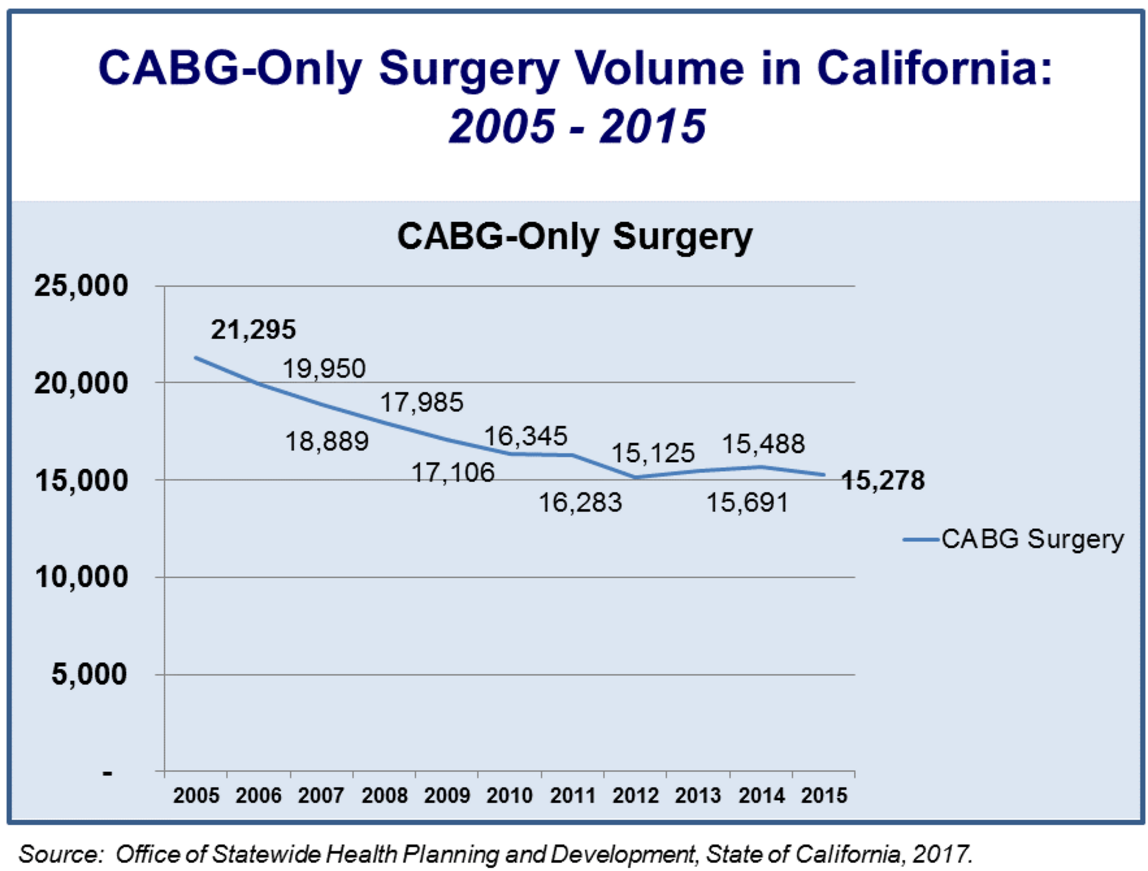
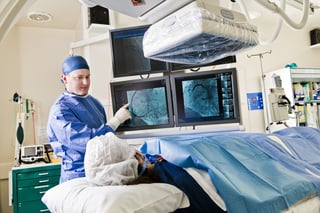 As we have reported in past blogs, California law now allows hospitals licensed to provide emergent cardiac catheterization laboratory services to perform scheduled, elective PCI regardless of the presence of cardiac surgery-on-site.
As we have reported in past blogs, California law now allows hospitals licensed to provide emergent cardiac catheterization laboratory services to perform scheduled, elective PCI regardless of the presence of cardiac surgery-on-site.